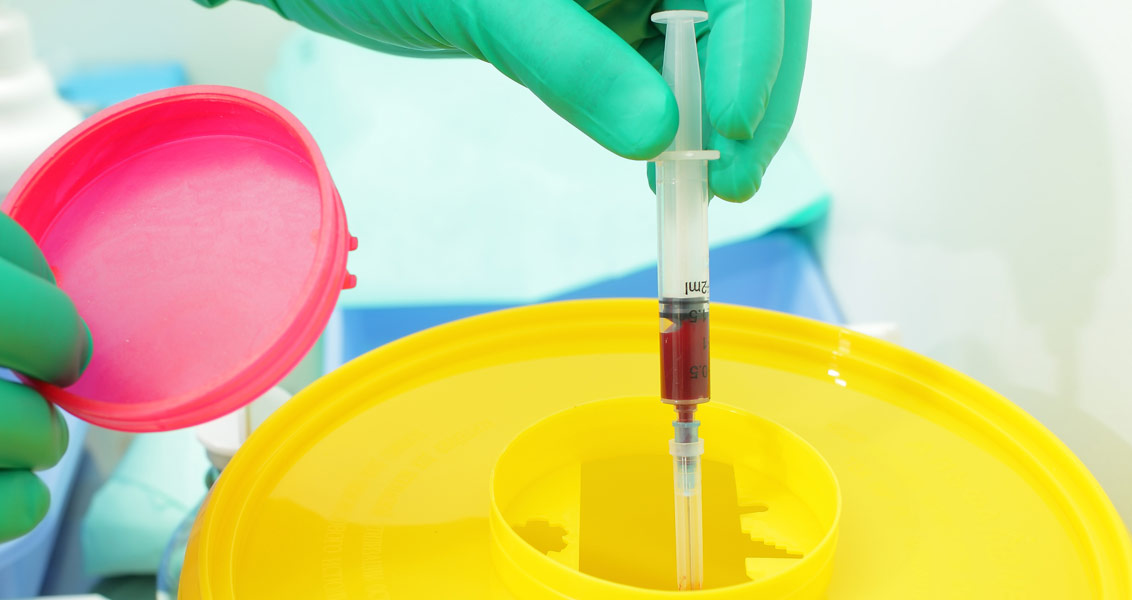

Injections are common drug delivery systems used in clinical practice and the needles and syringes are essential components of the modern healthcare services.
Syringes have a long history of evolution dating back to 17th century. However, there are different claims regarding the invention of a syringe by different individuals.
The forerunner of the modern syringe called the Fergusson syringe was first used by Alexander Wood in 1853. Opium was the first drug used to be injected for pain relieving.
Today, intravenous and subcutaneous administration of drugs is enabled using syringes. The concept of disposable syringes emerged as a technology since 1903 and evolved to the current state over the years, enjoying wide application, popularity and practical utility in the healthcare sector at a global level. They are in high demand as the need of injections are huge, especially in mass immunization drives, repeated/regular injections for chronic patients like diabetics, cancer patients, etc. However, the situation is same with drug abusers as well.
When and why syringe reuse happens?
In the developing countries, where affordable healthcare to the masses is still left unfulfilled; both patients and healthcare providers are either forced or tempted to opt for reuse of disposable syringes.
According to reports, there is an acute shortage of syringes among the developing countries, as the average number of daily injections in the developing world is about 17 billion.
Injections of controlled release drugs, mass application of the same drug in the hospitals, immunization projects, etc. are some of the situations where medical professionals opt for this risky process to overcome the shortage of syringes and or minimizing the cost involved.
The reuse of disposable syringes is one of the most common tendency observed across several countries. About 7 billion injections/year are reported as unsafe across the developing world.
The trend is not far from reality even in the developed world as cases of syringe reuse have been observed in Canada, USA, and other developed countries as well, but at a much lower rate. The syringes look pretty clean and often prompt the patients and the caretakers to change the needle and reuse.
What are the risks of syringe reuse?
Many blood-borne pathogens may enter the syringe via backflow during the injection process and contaminate the syringe since there is no classic way to prevent the entry of the pathogen into the syringe from the patient’s blood during injection.


Few consequences/case studies
Almost 39.3% of injections are given with reused syringes in the developing world. Grave incidences of transmission of blood-borne diseases have led to catastrophes in different parts of the world through unsafe injections.
According to a WHO report, unsafe injections account for 0.9% of deaths, 5% HIV infections, 24% cirrhosis cases and 28% of liver cancer on a worldwide level.
The case of Romania represents one of the massive calamities of the world with long-term impact. More than 10,000 children were contracted with HIV through unsafe healthcare in Romania, during the 1980s and the majority of them got infected by unsafe injections according to the reports.
Before this outbreak, there were only 13 adult cases of AIDS reported in this country and this catastrophe still accounts for over 50% of HIV infections among children across Europe since the discovery of this epidemic.
Hepatitis is the next most potent infectious disease spread through the means of unsafe injections. Almost one in five adults is infected by hepatitis C in Egypt from using unsafe medical Injections.
In fact, liver disease has turned to be a more important cause of death and disability in this country than the diseases the injections were targeted for. Every year, millions of new cases of hepatitis arise through unsafe injections worldwide.
What needs to be done?
Injections are life-saving medical intervention and saved millions of lives but they carry the risk of infections. “How to make injections more safe and beneficial in the developing nations?”, is a major concern for the modern healthcare service.
Different approaches for employing educational, managerial and regulatory parameters for ensuring safe and successful utilization of injections in the healthcare sector needs to be evolved.
Appropriate management and disposal of disposable syringes and following rational approach towards opting for injections for treatment can facilitate safe injection practice.
An honest commitment and diligent participation of the service providers, the patient community and the society in general supported by the policy makers can ensure safe injections. Focused social research to apprehend the problem in different parts of the world is required to evolve and implement evidence-based interventions.

Add Comment